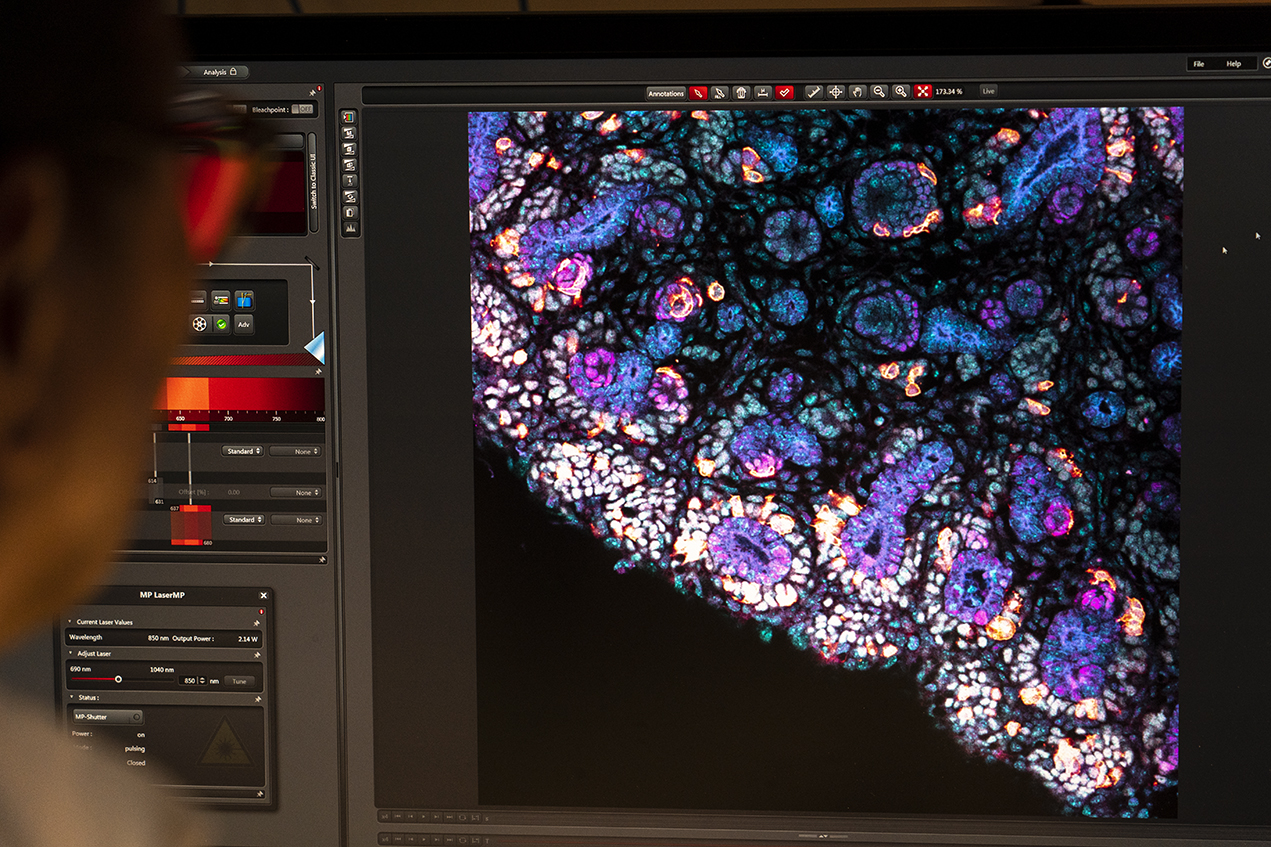
Developing new stem cell therapies requires more than a solo biologist having a eureka moment alone in the lab. Real progress relies on collaborations between biologists, engineers and physicians. That’s why The Eli and Edythe Broad Foundation has continued its support of two strategic initiatives: innovation awards bringing together teams of engineers and scientists from USC and Caltech, and clinical research fellowships for physician-scientists.
Engineering new approaches: The Broad Innovation Awards
For the fifth consecutive year, the Broad Innovation Awards are providing critical funding to USC-affiliated faculty members pursuing multi-investigator research collaborations related to stem cells. For the first year, these collaborations are also drawing on the expertise of biomedical engineers from Caltech. Each award provides $200,000 of funding for a one-year project.
With support from a Broad Innovation Award, Andy McMahon, PhD, the director of the Eli and Edythe Broad Center for Regenerative Medicine and Stem Cell Research at USC, is collaborating with Caltech biomedical engineer Long Cai, PhD, to leverage a new technology for understanding chronic kidney disease. The technology, called seqFISH, provides information about genetic activity taking place in intact tissue—enabling the study of the interactions between cells in their native environments.
“Dr. Cai’s seqFISH technology will provide an unprecedented insight into the cellular interplay underlying chronic kidney disease caused by a maladaptive response to acute kidney injury,” said McMahon, who is the W.M. Keck Provost and University Professor of Stem Cell Biology and Regenerative Medicine and Biological Sciences, as well as the chair of the department of stem cell biology and regenerative medicine at USC. “We aim to better understand this maladaptive response — which is more common in males —i n order to find new targets for preventing the progression to chronic kidney disease.”
A second Broad Innovation Award brings together USC Stem Cell scientist Rong Lu, PhD, and Caltech synthetic biologist Michael Elowitz, PhD. Their team will study the spatial organization of blood-forming stem and progenitor cells, also called hematopoietic stem and progenitor cells (HSPCs), which reside in the bone marrow. By pinpointing the locations of specific HSPCs, the scientists may find clues to explain why certain HSPCs are so dominant — replenishing the majority of the body’s blood and immune cells after a disruption such as a bone marrow transplantation.
“Spatial advantages may be the primary drivers of what we refer to as the ‘clonal dominance’ of certain HSPCs,” said Lu, assistant professor of stem cell biology and regenerative medicine, biomedical engineering, medicine, and gerontology at USC. “Understanding the spatial competition between HSPCs could help improve bone marrow transplantation and provide new insights into aging and the development of diseases such as leukemia — which are associated with clonal dominance.”
A third Broad Innovation Award brings together three collaborators at USC: Michael Bonaguidi, PhD, an assistant professor of stem cell biology and regenerative medicine, biomedical engineering, and gerontology; Robert Chow, MD, PhD, a professor of physiology and neuroscience, and biomedical engineering; and Jonathan Russin, MD, an assistant professor of neurological surgery and associate surgical director for the USC Neurorestoration Center. Their project focuses on finding new approaches to treating epilepsy by studying neural cells called astroglia. These cells perform a variety of key functions that support the health of neurons in the brain, and they may also play a role in modulating epileptic seizures.
“Although adults don’t tend to generate many new brain cells, humans do produce a limited number of new astroglia,” said Bonaguidi. “We will examine these newborn astroglia at the single-cell level to better understand their role in epileptic patients, and to lay the groundwork for identifying new treatments.”
The doctors are in: The Broad Clinical Research Fellowships
The Broad Clinical Research Fellowships are also entering their fifth consecutive year. These fellowships support stem cell research by physician-scientists and residents who intend to practice medicine in California.
“These fellowships provide a very special opportunity for our medical residents to engage deeply in laboratory research, as a complement to their extensive training in patient care,” said Laura Mosqueda, MD, dean of the Keck School of Medicine of USC. “This valuable research experience gives them a much more complete perspective on how to meet the challenges of finding the best possible treatments for their patients.”

A USC resident physician in general surgery, Kemp Anderson, MD, will spend his fellowship studying necrotizing enterocolitis, a very serious intestinal infection that affects nearly 10% of premature infants. Specifically, he will explore how a molecule involved in cellular communication, called farnesoid X receptor, or FXR, might contribute to this disease.
“If FXR plays a role in compromising intestinal barrier function in these premature infants, then altering the activity of FXR could potentially yield treatment modalities for necrotizing enterocolitis, avoiding the morbidity and mortality associated with surgical intervention,” said Anderson, who is performing the research under the mentorship of Christopher Gayer, MD, PhD, and Mark Frey, PhD, at Children’s Hospital Los Angeles (CHLA).

Brittany Rocque, MD, a resident physician in general surgery, will use her fellowship to seek better ways to predict, detect and diagnose immune rejection in patients who have undergone liver transplantation. Nearly 60% of pediatric patients and at least 15% of adult patients reject their liver transplants, and this can currently only be confirmed through an invasive surgical biopsy. Rocque is utilizing the technology “imaging mass cytometry” to identify and analyze the types of immune cells involved in rejection.
“My project has the potential to provide a noninvasive option to assess rejection in transplanted patients, and to expand our understanding of immune rejection,” said Rocque, who is being co-mentored by Juliet Emamaullee, MD, PhD, and Shahab Asgharzadeh, MD, at CHLA. “I’m greatly looking forward to applying my passion for transplantation surgery in the context of basic science, and enhancing my appreciation for the nuances of research, thanks to the Broad Clinical Research Fellowship.”

A hematology-oncology fellow who will be transitioning to a junior faculty position at USC next year, Caitlin O’Neill, MD, will study a condition known as “clonal hematopoiesis” or CH, a phenomenon common in the aging population. CH involves genetic mutations that cause the expansion of a particular population of blood cells without leukemia or related malignancies. CH increases risks for certain health conditions including heart disease.
During her Broad Clinical Research Fellowship, O’Neill will look at one mutation seen in patients with CH: a mutation to the gene called Tet methylcytosine dioxygenase 2, or TET2. O’Neill will explore if this mutation promotes blood clots, inflammation and heart disease.
“The goal is to inform therapies to prevent heart disease and leukemic progression in aging patients with CH,” said O’Neill, who is working with co-mentors Casey O’Connell, MD, and Lu at USC. “I’m very happy to be working on this project, with support from the Broad Clinical Research Fellowship, during my transition to becoming a faculty member at USC.”
— Cristy Lytal
This story has been edited for HSC News length and style requirements. Click here to read the original article in full.