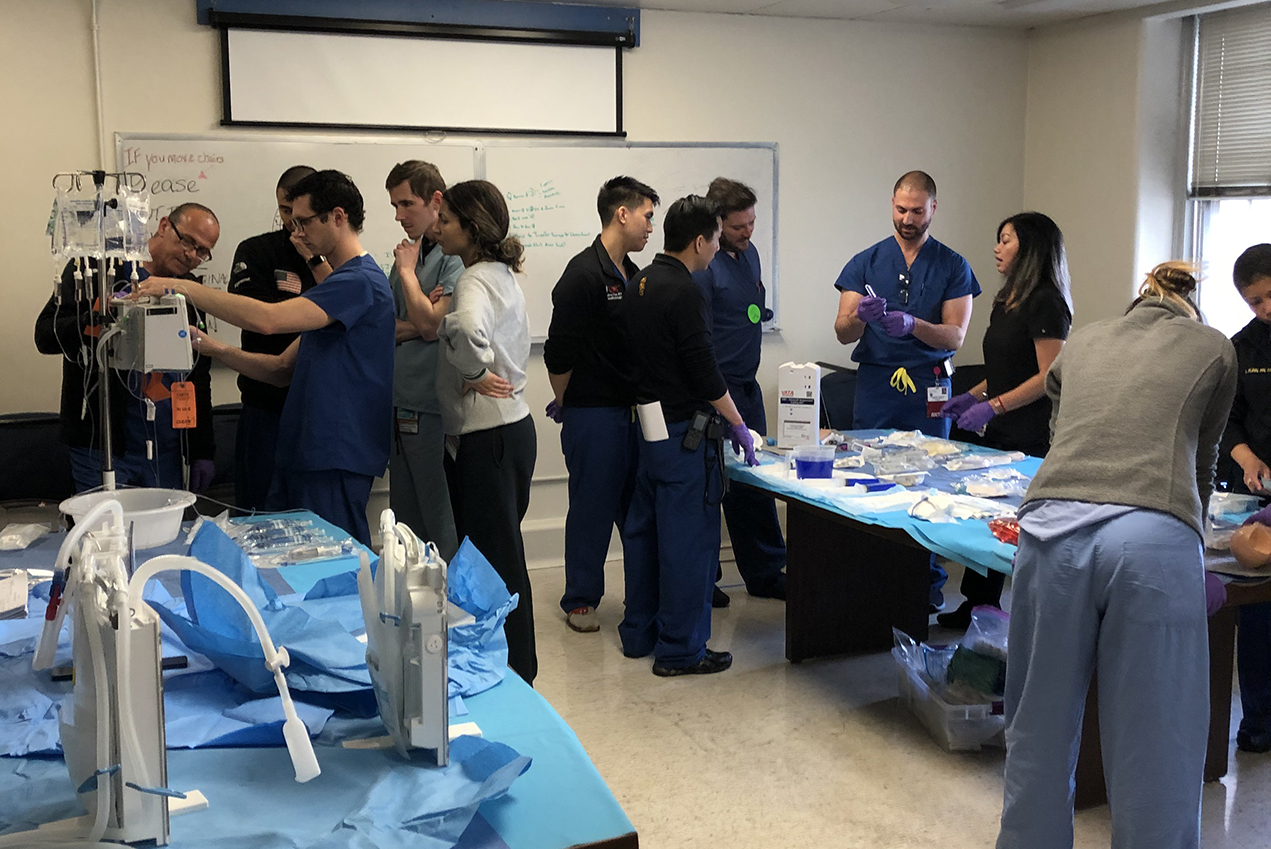
In response to the ongoing COVID-19 pandemic, caregivers across Keck Medicine of USC, LA County + USC Medical Center (LAC+USC) and the Keck School of Medicine of USC worked quickly to improve the response to this crisis. In an innovative move, trainers from LAC+USC held a series of workshops with surgical residents on Friday, March 20, to train them in vital critical care nursing skills.
“This is a supplement to their normal training,” said Meghan R. Lewis, MD, associate director of the LAC+USC Surgical ICU. “This will allow them to augment the critical care teams as we deal with the increased demand from this pandemic. We have a typical workflow and work patterns, but with the level of need we anticipate, there’s a lot of room for stepping in, especially with an overlap in skills. It’s time to look at things differently.”
Kenji Inaba, MD, chief of the division of trauma and critical care surgery at Keck Medicine and director of the surgical residency program at the Keck School, saw an early issue with surgical residents filling in for overburdened critical care nurses: “None of them, when we checked in, could hang an IV bag or adjust a ventilator. So Dr. Lewis put together a curriculum.”
Many people outside the world of health care think of doctors and nurses as having a great deal of overlap in their knowledge. That’s true to an extent, but as Maura Sullivan, PhD, associate dean of simulation education in health sciences at the Keck School explained, surgeons and critical care nurses have very different, highly specialized training.
“They’re all educated in medicine and patient care, but surgeons and nurses have roles that complement each other, so they have very different skill sets. Surgeons can’t just jump into a nurse’s role without some additional training.”
Sullivan, an experienced critical care nurse herself, was impressed with the adaptability of the residents.
“Our surgical residents are all smart individuals who just needed the training. Their attitudes were amazing. Everyone wants to help.”
Surgical residents learned skills such as performing blood draws, administering medication, setting up intravenous lines and handling the machinery of the ICU.
General Surgery Resident Christopher Foran, MD, said, “We give orders for things like titrating medicine and ventilator settings, but we don’t typically carry them out. This has been eye-opening for the residents. It has helped us all understand the nuances of ICU nursing care and gain a new appreciation of the work that critical care nurses do.”
The speed at which the special training came together was astonishing. Stephen Sener, MD, Chief of Surgery at LAC+USC, and Dan Donoho, MD, a chief resident of neurosurgery, came up with the idea on Tuesday and spoke with Lewis and Foran on Wednesday. The workshop was ready to go at 10 a.m. Friday morning.
Both Lewis and Foran had praise for the nurses who ran the training: Lieutenant Commander Lorelie Flinn, RN, MSN, CCNS, CCRN; Nofal Kahwaji, RN, MSN, CCRN; and Ramona Paolim, RN, CCRN; and for the Skills Center staff, Mike Minneti, Angela Martinez, and Dr. Maura Sullivan, who put the event together so quickly.
Kahwaji was pleased with how the workshop went. “This is a great example of the two disciplines taking their collaboration to a higher level. These surgical residents are taking a broader approach and stepping up to support the nursing staff if the demand requires it. I was delighted to see their level of engagement and eagerness to get this hands-on training. I hope this collaboration continues and spreads to other departments.”
The satisfaction with the workshop was mutual. “We feel much better prepared,” said Foran, “And this kind of training helps us stay adaptable. It’s easy to get into a one-track mind during your residency. There is a lot of value in going beyond what we have been doing every day.”
Lewis, an experienced acute care surgeon, agreed that this out-of-the-ordinary training would benefit the surgical residents in the long run: “This is an unparalleled experience. They will be more prepared for disaster-type scenarios for the rest of their careers.”
Both Lewis and Foran were all impressed with the readiness of the residents to adapt and jump into this new training.
“I’m incredibly proud,” said Foran. “This has brought out the best in our residents. Everyone raised their hands when we asked who wanted to do this. This is one more indicator that we have one of the best residency classes in the nation.”
“It’s been really impressive to see their eagerness to do this,” agreed Lewis, “They’re setting an example across departments. We’re hearing from residents and medical students everywhere that want to do this. This is about coming together to increase our capacity to care.”
In a heartening note, other medical schools have already heard about Keck Medicine’s innovative training for surgical residents and are eager to follow suit. Within days of the workshop, a resident at the University of Texas Southwestern Medical Center had contacted Dr. Inaba to request the curriculum to implement the training at their own center.
— Lex Davis