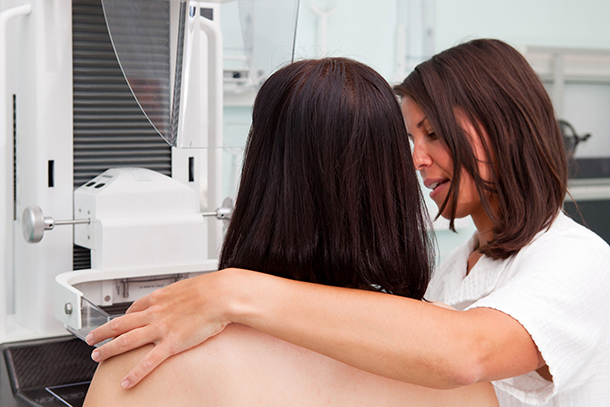
Asian women living in Los Angeles County are experiencing more breast cancer now than they faced nearly four decades ago, according to a recently released cancer report card administered by USC.
When compared to other Asian groups, Filipino women face the most breast cancer diagnoses in the county, but their risk is on the decline. The diagnoses went down 6 percent in the seven years between 2005 and 2012.
In contrast, Korean women are on the bottom of the list but are experiencing a steep and continuous increase in breast cancer rates, nearly quadrupling in the 32 years between 1980 and 2012.
The data comes from Cancer in Los Angeles County: Trends by Race/Ethnicity 1976-2012. Released on Aug. 15, the book is based on all cancers diagnosed among Los Angeles County residents over the past 37 years — more than 1.3 million cases.
Breast cancer is the most common cancer in women regardless of race or ethnicity and the most common cause of cancer death among Hispanic women, according to the Centers for Disease Control and Prevention. It is the No. 2 cause of cancer death among white, black, Asian and Pacific Islander women.
An estimated 246,660 women will be diagnosed with invasive breast cancer in 2016, and about 40,450 women will die from the disease this year, according to the American Cancer Society.
Christy Russell, MD, director of the Harold E. and Henrietta C. Lee Breast Center at the USC Norris Cancer Hospital and an associate professor of clinical medicine at the Keck School of Medicine of USC, has treated breast cancer patients for 30 years. Russell shares what has she gleaned from all that oncology experience.
Question: What causes breast cancer?
Christy Russell: Breast cancer is related to lifetime exposure of the breast tissue to uninterrupted estrogen and progesterone. The ovaries produce these hormones. Anything that prolongs the exposure to these hormones will increase a woman’s lifetime risk of breast cancer.
Once a woman begins her ovarian function during puberty, there are limited things she can do to reduce her risk of developing breast cancer. Interruptions in the menstrual cycle will reduce risk. The earlier and the more frequently she interrupts her menstrual cycle, the greater reduction in risk of breast cancer. This includes full-term pregnancy, prolonged breast feeding, steady and continuous physical activity, and maintaining a low and healthy body weight.
Q: When are most women diagnosed with breast cancer?
CR: Even though the majority of female breast cancer risk is established during the years between puberty and menopause, breast cancer generally occurs in older women. The median age for the appearance of breast cancer in women is mid-sixties.
Q: What role does alcohol play?
CR: More than 100 epidemiologic studies have consistently found that alcohol use is related to the risk of developing breast cancer, and there is no “safe” amount. The more alcohol consumed, the higher the risk.
After menopause, alcohol, higher body weight and hormone replacement therapy all increase the risk of breast cancer. These are all related to continued exposure of the breast to either estrogen alone or estrogen plus progesterone in the case of hormone replacement therapy.
Q: Although fewer Korean women develop breast cancer than any other ethnicity, their breast cancer risk has soared in the past 37 years. Why are more Korean women developing breast cancer?
CR: Presumably, they have taken on more “American lifestyle” choices, which would mean earlier puberty, later menopause, fewer pregnancies, less breastfeeding, perhaps less physical activity, higher body weight and possibly alcohol. Extensive epidemiologic studies need to be done to figure out which, if any, of these factors attributes to the rising rate of breast cancer risk in Korean women.
Q: If adopting a more American lifestyle could be the culprit, why has the rate of breast cancer among white and black women begun leveling off in the past decade?
CR: The risk of breast cancer in white and black women is likely leveling off because of their steady use of screening mammography. Additionally, during the time frame when their risk of breast cancer is developing, they probably continue to have similar lifestyle habits as those in years past, such as age at first full-term pregnancy, length of breastfeeding, use of hormone replacement therapy, exposure to alcohol and total body weight.
Q: Girls are reaching puberty earlier nowadays — sometimes starting at age 8. What does early puberty mean for breast cancer risk?
CR: Initiation of puberty is related to a young woman attaining a specific height and weight. Presumably, the body knows when it is capable of childbearing and thus puberty begins. Populations in the world with greater health and nutrition during childhood will decrease the age at which their girls start puberty.
Reaching puberty earlier increases the amount of estrogen and progesterone a young woman receives in her lifetime, so earlier puberty increases her risk of developing breast cancer.
Q: Should menopausal women abstain from hormone replacement therapy to limit their breast cancer risk?
CR: The use of hormone replacement therapy is a very personal decision and should be based on the extent of menopausal symptoms such as hot flashes, sweats and sleep disturbance. The use should be limited in terms of number of years and should be discontinued as early as possible to reduce the subsequent increased risk of breast cancer. The longer a woman is exposed to hormone replacement therapy, the greater her risk of developing breast cancer.
However, that being said, the majority of breast cancer risk is related to one’s lifetime exposure to estrogen and progesterone and is not just related to what happens after menopause.
— Zen Vuong