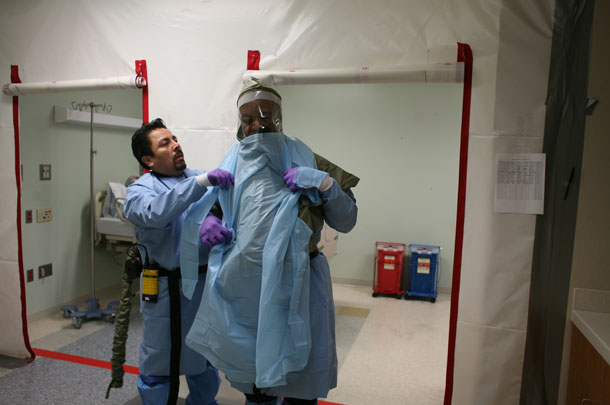
It starts with selected hospital scrubs that are impermeable to fluids and cover the torso, arms and legs.
Next come booties for the feet and ankles that extend to mid-calf. A fluid-resistant gown follows. Then a battery-powered air purifying respirator (PAPR) is deployed, attached to a hood with a full face shield and a protective cowl to cover the neck and shoulders. The process concludes with medical gloves – two pair, in fact. When finished, no skin is left exposed.
Donning the equipment takes a good 15 minutes; getting out later may take 30 minutes more.
At Keck Medical Center at USC, 87 health-care professionals recently volunteered to learn this dressing ritual. They were learning to protect themselves in the event an Ebola case was identified.
When an outbreak of the deadly Ebola virus in West Africa began making headlines last September, personnel at Keck Medical Center sprang to action. Within a few weeks, Stephanie Hall, MD, and a team of physicians and nurses led by Emergency Management Officer Robert “Bob” Vance III and Infection Prevention & Control Manager Lionel Caceres, RN, and his infection prevention team had instituted a training program to ensure that medical personnel would be knowledgeable about working with the disease and fully prepared to take action should someone arrive in need of treatment.
The mission is to “detect, protect and respond,” Caceres says about the medical center’s role in dealing with the Ebola crisis. Any person identified at a Keck Medicine facility would be transferred in coordination with Los Angeles Public Health as soon as possible to one of the treatment centers designated by the Centers for Disease Control (CDC).
Three single-patient training rooms with a closed door and a private bathroom rooms were created at Keck Hospital of USC. Then volunteer physicians and nurses began two-day training sessions, starting soon after the CDC issued new wrinkles in recommended procedures in mid-October. Ebola-related screening questions were added to the patient triage process a few weeks later.
The use of the special gear, known as personal protective equipment (PPE), is necessary when dealing with Ebola, which is spread through direct contact with body fluids of a person who is sick with the disease. But it can be difficult for trainees to abide by the painstaking process of donning and doffing the gear. Not everyone completes the training successfully.
“It’s difficult,” Caceres says. “Human behavior is such that you want to hurry up and help the patient, but this is not that kind of situation. You need to protect yourself first.”
Getting into the PPE is a two-person process, and the training partners must stay together throughout. It’s difficult to hear inside the PPE, so hand signals are necessary inside a treatment room to ensure effective communication. Strict guidelines must be followed, particularly when disrobing afterward, which includes disinfection and hand-washing at each level.
In an actual treatment scenario, a patient floor at Keck Hospital would be isolated and converted for treatment within 8-12 hours. The two-person teams of health-care workers would treat a patient in shifts that would last no longer than two hours at a time. And they would be responsible for ensuring that anything that goes into the patient’s room gets disposed of as a biohazard afterward.
“So, no cellphones, no rings or watches. Don’t wear your favorite pair of Nikes — they will be disposed of too,” Vance says. “You cannot cut corners with this disease.”
Protecting the body is just one aspect of the training regimen. Health-care workers must train their minds as well.
“Training includes an isolation aspect,” Vance says. “This process allows our staff to reduce the level of fear that might occur during treatment.”
The experience has been valuable for staff members who may have to contend with outbreaks of another deadly disease in the future. And the Ebola effort is not complete. The training rooms are permanent, and follow-up sessions are taking place, as are surprise drills to validate the procedures.
The Ebola response at Keck Medical Center of USC has been extensive, involving numerous hours of research, documentation and training, construction of appropriate facilities and purchase of new equipment.
“It’s a large expense. This is not cheap,” Vance says. “But the medical center is making an investment in its employees and wants them to be safe.”
— Les Dunseith