Your smartphone could be the key to a healthy heart.
At least that’s what Niema Pahlevan, PhD, believes. The 39-year-old engineer has been developing an app that could allow people to use their iPhone camera to measure heart health. The high-tech, low-cost tool would address America’s No. 1 cause of death: heart disease.
About 790,000 Americans have a heart attack every year, according to the Centers for Disease Control and Prevention. That amounts to a heart attack every 40 seconds.
“This app doesn’t exist in the market yet, so people don’t know they need it,” said Pahlevan, assistant professor of aerospace and mechanical engineering at the USC Viterbi School of Engineering. “Nearly 50 percent of heart attacks are silent — the heart is damaged, but people aren’t aware they just had a heart attack. So they don’t seek treatment to prevent future heart attacks. We are working to help doctors and our future app users identify silent heart attacks and, really, any heart failure before they happen.”
Heart attacks typically cause chest pain or other warning signs such as shortness of breath, cold sweats, nausea or lightheadedness. But silent heart attacks either do not manifest these symptoms or people misinterpret them. As a result, the condition usually goes untreated, tripling the chances of death from heart disease, according to a 2016 study by the American Heart Association.
A seasoned engineer of noninvasive diagnostic methods and devices, Pahlevan is among a handful of rising scientists who recently moved their labs into Michelson Hall on the University Park Campus. The USC Michelson Center for Convergent Bioscience is a place where scientists, engineers and medical professionals work collaboratively to solve some of the greatest intractable problems of the 21st century in biomedical science, from fundamentally new understanding of the cell to new approaches for cancer, neurological and cardiovascular disease.
Sending real-time health data to doctors
To measure the heart’s pumping efficiency each time it contracts, patients generally obtain a cardiac MRI, echocardiogram (heart ultrasound) or CT scan. Alternatively, they undergo an invasive procedure that requires a catheter to be inserted into an artery in either the groin or arm. These are time-consuming procedures and require expertise from cardiologists, trained technicians and nurses. Additionally, they are performed only when there is an obvious need for them.
“Having heart failure or experiencing a heart attack is not on anyone’s bucket list,” Pahlevan said. “Heart failure doesn’t happen overnight. Sometimes it happens over many years, so having the ability to use your iPhone to conveniently observe heart health over a prolonged period empowers you and your doctor to identify if you’re on the road to heart failure.”
Preventive measure
The algorithms and app Pahlevan and his colleagues have been working on are a form of preventive medicine. This biotech solution can also keep an eye on heart failure patients. People can spend as little as a couple of seconds to get a complete reading via this diagnostic tool, Pahlevan said.
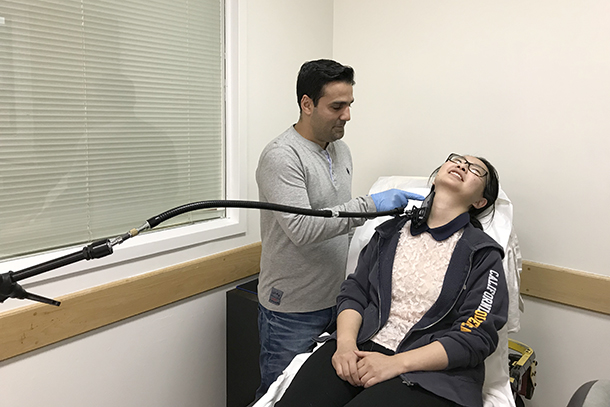
All the user needs to do is place an iPhone camera or, eventually, any smartphone camera against their carotid artery pulse on the left or right side of their neck. These major arteries provide blood to the brain, neck and face.
The camera records the vibration of the blood vessel and provides a wave curve that contains information about how much blood the heart is pumping out per contraction. (The researchers developed a cradle to eliminate inaccurate results due to shaky hands.) If the percentage of blood that exits the heart (ejection fraction) is 50 to 70 percent, the heart is healthy. Anything below 45 percent signifies subpar blood delivery and heart failure, Pahlevan said.
Proof that the app works
Pahlevan led a study published in the journal Critical Care Medicine this summer that found the iPhone diagnostic app his team created was slightly more accurate than an echocardiogram, the most common technique employed in clinical practice to identify heart failure.
The study included 72 study participants, both people with and without heart failure. Notably, the tool’s accuracy was stronger among heart failure patients, a population in need of more precise and timely heart health diagnostic tools.
“The algorithm we created computes the biomarkers for heart failure and, eventually, heart attacks,” Pahlevan said. “The percent of blood pumped in each heartbeat can be sent to a cardiologist who will then, for the first time, have a real-time record of the patient’s heart health over a critical period.”
Extending the technology to other spheres
Now that Pahlevan has a proof of concept, his iPhone app has piqued the interest of many researchers and even the biotech industry. He is working with Keck Hospital of USC to test a more advanced algorithm that uses information received from an iPhone camera and electrodes attached to the chest.
The electrocardiogram cannot measure “left ventricular end diastolic pressure” (LVEDP), the most robust biomarker of whether a person’s heart is pumping normally. He is collaborating with Ray Matthews, MD, professor of clinical medicine at the Keck School of Medicine of USC and director of USC Interventional Cardiology and Catheterization Laboratories, and his team at Keck Hospital of USC to demonstrate the proof of concept of a new theory that allows measuring LVEDP using an iPhone.
Once the tool is fully tested, people will be able to place a smartphone against their neck pulse and attach two electrodes to the skin of their chest to get an accurate reading of their heart health. All the information will be input into their smartphone app and sent to their physician or cardiologist. This can be done from the comfort of their home, without disrupting their day.
“The initial tool we created for ejection fraction is like a bicycle, and this new tool we’re working on is like a Ferrari,” Pahlevan said. “You can get there much sooner, much faster.”
Smart algorithm
Extending into a slightly different realm, Pahlevan is also working on an algorithm for a smartphone app that could serve as a diagnostic tool to identify people who are at higher risk of dementia and Alzheimer’s disease. Cardiovascular disease has been associated with the memory-erasing disease.
As a research institution devoted to promoting health across the life span, USC has more than 70 researchers dedicated to the prevention, treatment and potential cure of Alzheimer’s disease.
Pahlevan has received funding through equity and consulting work from a biotech company developing his heart health technology for market. Derek Rinderknect, Peyman Tavallali and Marianne Razavi from the biotechnology company Avicena; Thao Tran and Marie Csete from Huntington Medical Research Institutes; Michael Fong and Robert Kloner from the Keck School of Medicine of USC; and Morteza Gharib from Caltech contributed to the study published in Critical Care Medicine in July.
— Zen Vuong